Doctor in the morning, researcher in the afternoon Inspire article
For doctor Stefan Pfister, efforts to cure cancer happen at the hospital and in the laboratory.

Pfister works is quite
colourful – some doors
even have stickers on
them. No wonder: it is a
hospital for children.
Image courtesy of the DKFZ
Professor Stefan Pfister is a medical doctor who looks after children suffering from cancer. However, he and his colleagues are not always in a position to help. Sometimes cancers continue to grow in spite of all possible treatments. Unwilling to accept this, Stefan became a researcher as well as a doctor. In the afternoon, he changes from his doctor’s coat into his laboratory coat and searches for potential methods of making cancerous cells harmless.
When Stefan walks through the corridors of the paediatric clinic in Heidelberg, Germany, one can hardly keep up with him. The 38-year-old specialist in childhood cancers is in a hurry to reach his patients. Today Stefan is on duty in the outpatients department. His first patient is Felix.* “Felix is 5 years old and has leukaemia,” says Stefan. “That is the most common type of cancer among children.” Leukaemia, which means ‘white blood’ in Greek, occurs when white blood cells, the leucocytes, suddenly begin to multiply at an inordinately rapid rate. These cells normally combat bacteria and other pathogens, but when there is a surplus of leucocytes, they can no longer function properly. As a result, a minor infection can be life-threatening. “For that reason, we are treating Felix with chemotherapy. It fights the cancerous cells in his blood.” However, the medication damages healthy cells as well. Stefan therefore has to take a blood sample and perform the blood count to gauge the effectiveness of the treatment. A little later, the results are in. “Felix is lucky,” says Stefan, who is pleased that his young patient “has a sufficient amount of healthy cells in his blood”. That means Felix does not need to stay in the clinic and is allowed to return home with his mother.

Centre in Heidelberg,
called Angelika-Lauten-
schläger-Klinik.
Image courtesy of 2micha
Wikimedia commons
In the room next door, the next patient is already waiting. “Alexander* is 10 years old and has a tumour growing in his head,” says Stefan. “If the tumour becomes too big, the pressure in Alexander’s head will increase and vital nerves could be squashed.” To prevent this from happening, Stefan’s colleagues, the neurosurgeons, removed a part of the tumour some time ago – in a very complicated operation. Today, Stefan would like to take pictures of Alexander’s head with the help of a magnetic resonance imager, or MRI for short.
“On these MRI pictures I can detect whether the tumour has begun to grow once again.” Although the examination is not painful, Alexander has to lie motionless for half an hour in a narrow tube. He is very frightened of this, and so receives a sedative beforehand to induce sleep.

way from the paediatric
clinic to the German
Cancer Research Centre. He
usually goes by bicycle,
even when it’s raining.
Image courtesy of the DKFZ
On this day, many other children arrive together with their parents at the outpatients department. Stefan takes blood samples almost non- stop, listens with his stethoscope to respiratory and cardiac sounds, and replies patiently to questions asked by children and their parents. At lunchtime he picks up his own 6-year-old daughter from school and brings her to the after-school day centre. Then he devotes his time to his patients once again. “We can save a lot of children by means of an operation, chemotherapy or radiation treatment,” says Stefan.
“Nonetheless, sometimes the cancer continues to grow.” He just cannot come to terms with this, and so on some days Stefan not only visits the hospital but also makes his way to the German Cancer Research Centre (DKFZ) in Heidelberg. There, he examines cancerous cells in the laboratory with the aim of finding a way to make them non-harmful. However, today Stefan has to stay a little longer in the hospital: Alexander has finished with his MRI examination, but he is still asleep. Until the sedative wears off, a medical doctor must remain nearby. When Alexander wakes up, Stefan enquires how he is. “A little tired, but otherwise fine,” Alexander replies. Stefan is relieved and heads off to the laboratory.
An international effort
When Stefan Pfister hops on his bike to cycle to the DKFZ, it is already dark outside. If you imagine a researcher sitting over a microscope in his white coat or pottering around with test tubes, you would be right sometimes. On this particular evening, however, Stefan’s research tools are restricted to a computer and a telephone, as a teleconference is on the agenda. He and his laboratory colleagues in other countries will discuss their recent research findings. By doing this, they can learn from one another and can make quicker progress with their research. It goes without saying that such an international collaboration will take place in English.

Stefan and his team at the DKFZ are interested in the genetic composition of cancerous cells. “The genetic make-up contains all the information on the tasks of such a cell, its appearance and when it should act,” the scientist explains. The genetic information contained within DNA is located in the core of almost every cell. One can imagine it as being like a book that is written using only four letters. “Cancerous cells have such a book – but they always have some spelling mistakes,” explains Stefan. “By means of special devices called DNA sequencers, we can read these books and look more closely at single chapters, the so-called genes.”
In the DKFZ, ten sequencers stand in a room of their own. “We use these to examine not only the cancerous cells but also healthy cells,” Stefan explains. “Afterwards we can compare them on the computer and see how a cancer cell differs from a healthy cell – in other words, find the spelling mistake in the text. If we can then understand which chapters have been changed, we can perhaps develop new and better medication against cancer.”
Traces in the cerebrospinal fluid
Currently Stefan and his colleagues are examining, among other things, the cerebrospinal fluid. “This is a fluid located in the brain, but also found in a canal in the spinal cord,” explains Stefan. “When somebody has a tumour, in most cases single cancerous cells also float in the cerebrospinal fluid – even when the tumour is very small.” Because the fluid can be extracted from the spine with a needle, researchers can search for traces of such cancerous cells, or, to be more specific, damaged genetic material. If they detect cell damage in the cerebrospinal fluid, then it is obvious that the patient has a brain tumour. Applying this method will enable researchers to detect whether a tumour has disappeared during treatment. For example, should the doctors locate cancer cells in the cerebrospinal fluid, they could then treat the patient for a longer period and more intensively.“We now want to find out if that works,” says Stefan.
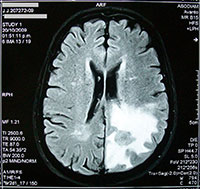
tumour
Image courtesy of Bobjgalindo
Wikimedia Commons
Some children are already benefiting from Stefan’s research. An especially malignant form of brain tumour, for example, can be separated into one of three different classifications. As a result, some patients can now be healed with less intensive therapy, because it is known that their tumours respond very well to therapy. Stefan has won many awards for this discovery, but they are not so important to him. What matters far more, he says, are the benefits that his small patients can reap. “I am so pleased every time we discover something that can help them.”
This article was adapted from an article that first appeared in Einblick, published for children by the DKFZ
*Names have been changed
Review
The medical practitioners who carry out innovative research in their field have a valuable insight into the potential of new treatment. The article gives an overview of a day in the life of one such person, Professor Pfister. All cancer cells have alterations in their DNA sequences. What exactly are these changes in a particular cancer? This is the subject of ongoing research with a good deal of progress being made, including by Professor Pfister, so that medication can be tailored to target the cancer cells.
This article can be used in several ways. It introduces DNA and the value of DNA sequencing within a medical context. For the 14-16 year old age group it could be linked to DNA structure and gene expression and what happens when DNA changes. They could also look at different types of leukaemia, chemotherapy (such as monoclonal antibody treatments) and immunity. This could be extended for the 16-19 age group into the theory of DNA sequencing and an extension activity on molecular biology, the value of the Human Genome Project and proteomics. The MRI scanner could be investigated within medical physics. Finally, the article could be used in lessons on moral and ethics to start a discussion on cancer therapy, whether it is right to only trial treatments on the sickest patients, the value of palliative care and hospices and perhaps extended into the tricky subject of euthanasia.
Shelley Goodman, UK





